Brain imaging links stimulant-use relapse to distinct nerve pathway

You might assume that people who are most prone to developing a substance use disorder in the first place would also have the hardest time avoiding relapse following treatment. But a new study by scientists with the Wu Tsai Neurosciences Institute’s NeuroChoice Initiative reveals that relapse may be linked to quite different brain circuits than addiction itself.
“There’s a huge revolving door problem with relapse,” said Brian Knutson, a professor of psychology. “These findings suggest that what gets you into taking drugs may not be the same processes that get you out of it, which could be very valuable to help predict who is at highest risk of relapse coming out of treatment.”
Drug addiction presents a major global challenge. More than 35 million people worldwide self-report problematic use of drugs and admissions to drug treatment programs have surged in the United States in recent years. For many drugs, in particular stimulants such as cocaine and amphetamines, relapse remains a common problem. For example, as many as 50 percent of people with stimulant use disorders relapse within 6 months of release from treatment.
“The statistics are disheartening,” said Kelly MacNiven, a social science research scholar in the Knutson lab and co-author of the new study. “Unfortunately not much is known at a biological level about the drivers of relapse — understanding this better is going to be the first step to developing better ways to help people get out of dependence.”
Our thoughts and behaviors arise from rapid electrical and chemical interplay between dozens of specialized centers within the brain. One structure found deep in the middle of the brain called the nucleus accumbens plays a particularly important role in addiction. This structure can be thought of as assessing the value of our actions based on the rewards they reap — measured in the currency of the neurotransmitter dopamine — and strengthening circuits that motivate us to repeat the most valuable actions. By artificially triggering huge release of dopamine, drugs of abuse immediately juice motivation — eventually burning an artificially high value on drug-seeking behaviors into the circuit. These deeply carved neural pathways can be extremely difficult to unlearn despite many negative consequences.
Researchers used advanced brain imaging techniques to study nerve fibers connecting to the nucleus accumbens, which plays an important role in motivation and addiction. Credit: Loreen Tisdall and Kelly H. MacNiven.
But of course not everyone is equally susceptible to developing substance use disorders, which Knutson and others believe has to do with differences in the details of the complex brain circuits in which the nucleus accumbens is embedded. But only recently have advances in brain imaging technology made it possible to measure these fine differences in human patients.
For example, MacNiven and her Knutson lab colleagues recently showed that the strength of connections from midbrain dopamine neurons to the nucleus accumbens is linked to individual differences in impulsivity — how much people value immediate over larger future rewards — as well as people’s risk of developing addiction. Notably, the brain differences that predicted diagnosis with stimulant use disorder did not map onto patients’ success avoiding relapse after treatment.
“This was an early hint that something different might be going on in the brain when people are trying to avoid getting back into drug use,” Knutson said. “This is in part what motivated us to look deeper into the circuitry underlying relapse.”
In their new study, published June 20, 2022 in the journal PNAS, former Knutson lab member Loreen Tisdall, MacNiven and colleagues used MRI scans to measure the fine structure of nerve tracts linking various brain structures to the nucleus accumbens in 60 people enrolled in treatment for stimulant use disorder. They then followed these patients for six months after treatment to see whether those who ultimately relapsed might show particular differences in the brain circuitry of addiction.
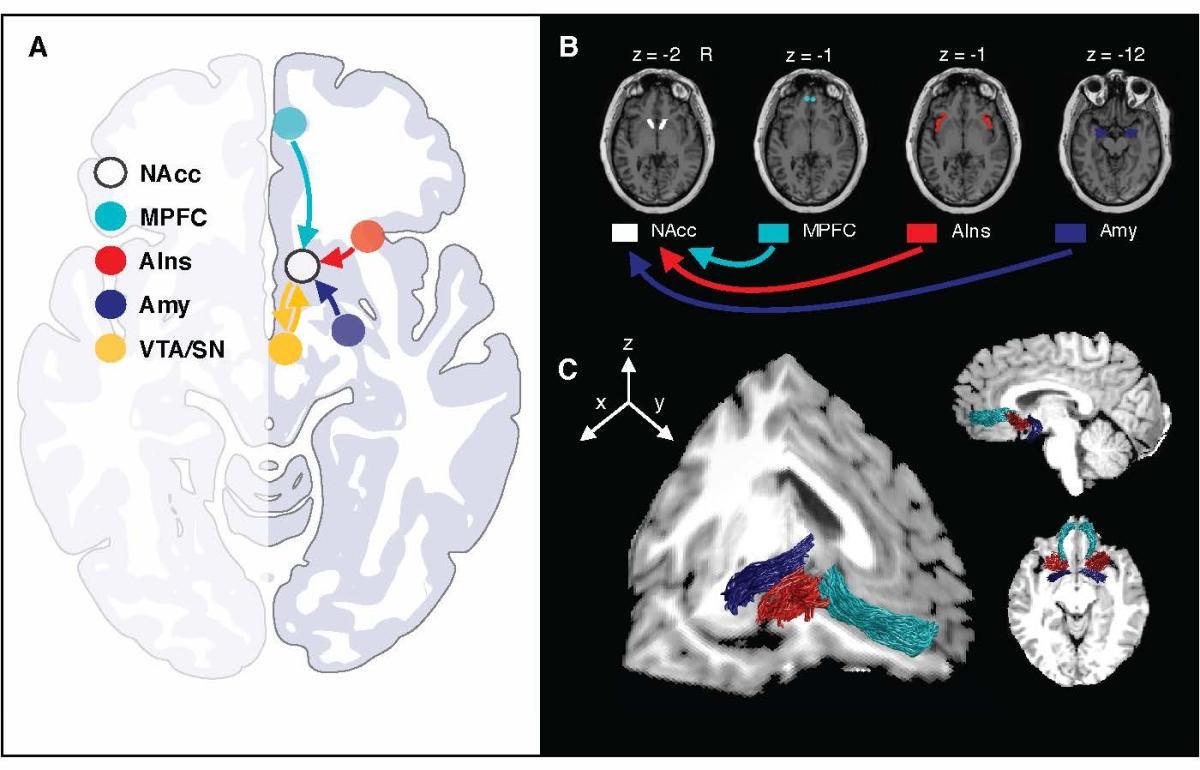
Researchers characterized multiple nerve tracts converging on the nucleus accumbens (NAcc) in humans, shown here in a representative subject. Light blue: medial prefrontal cortex (MPFC); red: anterior insula (AIns); indigo: amygdala (Amy); yellow: midbrain dopamine neurons (VTA / substantia nigra). Credit: Loreen Tisdall and Kelly H. MacNiven.
Based on this data, they found that patients who relapsed within six months showed weaker anatomical connections to the nucleus accumbens from an area called the anterior insula, which has seen a flurry of interest in recent years as a center for alertness and self control. In fact, Knutson’s lab had recently shown in healthy volunteers that the anterior insula to nucleus accumbens connection is associated with the ability to inhibit ongoing behavior – particularly when large incentives are at stake.
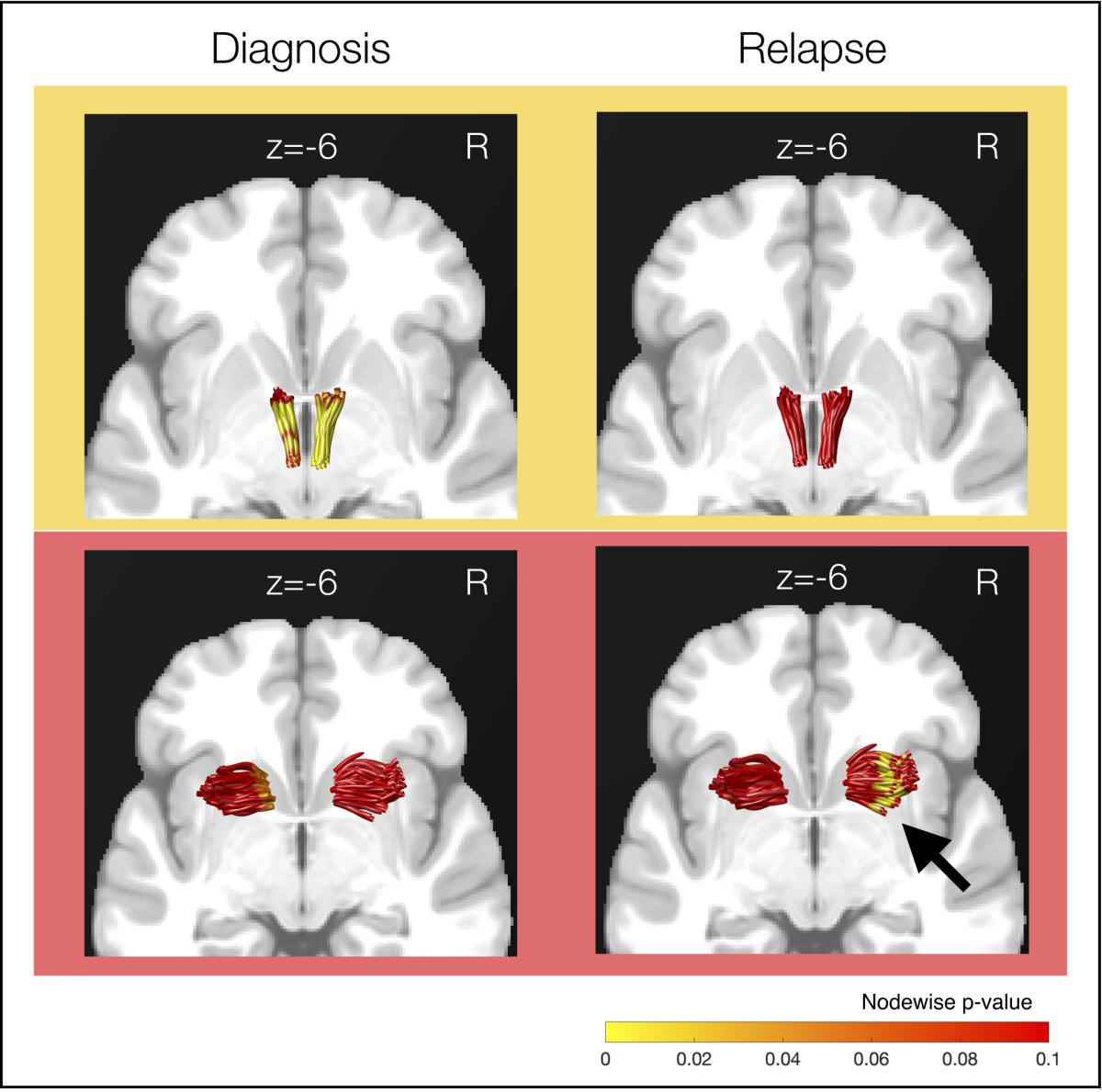
The strength of nerve fibers linking midbrain dopamine neurons to the nucleus accumbens were linked to stimulant-use diagnosis but not to relapse (top row), while the strength of anterior insula to nucleus accumbens fibers were linked to relapse but not diagnosis (bottom row). Credit: Loreen Tisdall and Kelly H. MacNiven.
“These findings are exciting because they suggest that we could meaningfully predict which individuals are likely to struggle most to avoid relapse following treatment, and potentially devote more resources to helping them build resilience,” Knutson said.
“We also suspect that the strength of neural pathways such as this can be altered with training and experience,” MacNiven added. “This will require more study, but there’s potential that understanding the pathways involved in relapse could lead to the development of targeted interventions to strengthen these pathways.”
The findings grew out of the NeuroChoice Initiative, a Wu Tsai Neuro Big Ideas in Neuroscience research program that set out to link extensive animal research into the brain mechanisms of decision making with actionable human neuroscience and policy research in the realm of addiction.
Human brain imaging has always been limited, compared to animal research, by its relatively low resolution — making it difficult to discern the fine variations in nerve fibers that make one brain different from another. But advances in the technology and analytical techniques in recent years are shrinking this gap.
Diffusion-weighted MRI (also known as diffusion tensor imaging, or DTI) maps the paths of nerve tracts through the brain based on how these microscopic tube-like structures conduct or block the flow of water molecules.
With support from NeuroChoice, MacNiven and co-author Josiah Leong spent years developing new computational techniques to improve the ability of so-called diffusion MRI to discern the delicate warp and weft of small nerve fibers that criss-cross the human brain.
“Previously these techniques were able to trace the superhighways of the brain — major nerve bundles like the corpus callosum that are easier to identify .” MacNiven explained. Now she and colleagues can accurately map much finer-grained nerve tracts whose paths can vary dramatically from person to person — more akin to the winding old roads that give a city center its unique character.
“The long-term funding Neurochoice provided was also critical to be able to recruit and follow these patients during and after treatment,” Knutson added. “We began this project in 2015, so the commitment Wu Tsai Neuro made to seeing this work through was absolutely critical.”
Within five to 10 years, Knutson predicts, clinicians will be able to use measures of brain structure to identify which patients coming out of treatment will likely benefit most from additional interventions to help them avoid relapse. These measures may also be valuable to develop focused interventions using psychotherapy, pharmacology, or even targeted brain stimulation to help strengthen key pathways and enhance the brain’s resilience.
The study’s lead author was Loreen Tisdall, now at the University of Basel in Switzerland. Additional authors were Claudia Padula of the VA Palo Alto Health Care System and Josiah Leong, now of the University of Arkansas. Brian Knutson is a professor in the Stanford Department of Psychology and a member of Stanford Bio-X, the Institute for Human-Centered Artificial Intelligence (HAI), the Stanford Woods Institute for the Environment, and the Wu Tsai Neurosciences Institute.
This research was funded by the NeuroChoice Initiative of the Wu Tsai Neurosciences Institute and a P50 center grant from the National Institute of Drug Abuse.